X
Practical review of genital herpes symptoms: frequency and progression, initial outbreak and flare-ups, photos and statistics.

By Slava Fuzayloff | Published on May 31, 2023

PART 1
What are the symptoms of genital herpes infection?
The symptoms of a herpes outbreak include prodrome symptoms and a skin rash.
What does “prodrome” mean?
In about 24% of cases, herpes flare up accompanied by systemic symptoms. Systemic symptoms are the ones that affect the whole organism such as:
- Fatigue
- Lack of appetite
- Body aches
- Fever
- Chills
- Other flu-like symptoms.
People start having systemic symptoms with herpes flare up as early as 12 hours after initial exposure.
It is more common to have systemic symptoms with first outbreak.
Herpes skin rash
A herpes skin rash evolves over time and can present as redness or a blister, sore, or crusted sore.
How common are herpes symptoms?
Around 70-80% of infected people do not have disease-related symptoms or the symptoms are rather mild to be noticed. Immune system of most people is strong enough to keep the virus suppressed, in the latent stage. It is important to remind that once herpes contracted it stays with the person for life. Occasionally immune system might go down and symptoms might show up.
The list of triggering factors that lead to the latter outcome includes but is not limited to:
- Stress
- Trauma
- Illness
- Menstruation
- Surgery
However, the chance of having herpes symptoms goes down over time. Herpes is the regressive condition- lesser chance of outbreak as the times goes on.
Time from herpes simplex virus exposure to having symptoms.
Again, about 70%–80% of infected people never get symptoms of herpes. Among symptomatic patients, the symptoms may appear as early as 12-24 hours after exposure. However, the majority of people develop symptoms 2-12 days after being infected. [1] Genital Herpes – CDC Detailed Fact Sheet https://www.cdc.gov/std/herpes/stdfact-herpes-detailed.htm
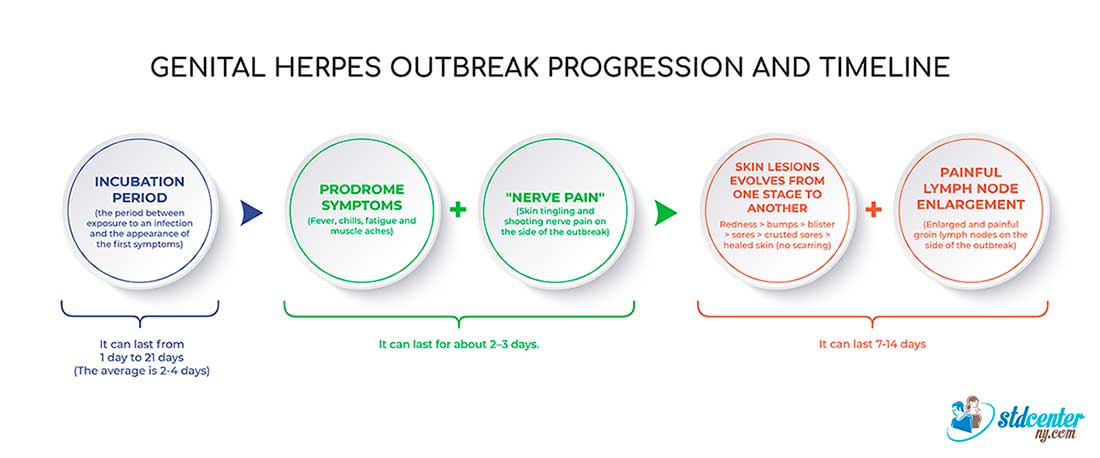
How do herpes symptoms progress?
Stage 1:
A symptomatic patient begins to experience a tingling or itching sensation in the area of exposure 12–24 hours after initial herpes exposure. In addition, systemic symptoms such as fever, fatigue, and headache might occur. [2] Kimberlin DW, Rouse DJ. Genital Herpes. N Engl J Med, 2004. 350(19): 1970–7. https://www.nejm.org/doi/10.1056/NEJMcp023065
Stage 2:
Herpes-specific blisters develop in the affected areas. There are multiple blisters clustered on a red base.
Blisters almost always appear after stage 1 in symptomatic patients.
Occasionally, symptoms don’t progress to signs because the immune system acts fast, suppressing the outbreak, or because the person is taking herpes-suppressive medication. This usually happens with flare-ups: the virus reaches the surface and the skin become infectious, but no signs of herpes appear.
In the first outbreak, it can take 2–12 days (the average is 4 days) before lesions appear; in subsequent outbreaks, skin blisters can appear as soon as 12 hours after stage 1.
Stage 3:
The blisters break within 7 days of appearing and leave aching ulcers or sores (which may bleed).
Stage 4:
Once ulcers develop, healing takes about 1–4 weeks. Scars don’t develop. The time is longer (2–4 weeks) for newly infected people and shorter (1 week) for people experiencing a recurrence. [2] Kimberlin DW, Rouse DJ. Genital Herpes. N Engl J Med, 2004. 350(19): 1970–7. https://www.nejm.org/doi/10.1056/NEJMcp023065
The symptom can be very subtle and very short-lived that most people do not notice the progression of symptoms.
Symptoms severity and progression may be different each time and depends on the competency of immune system at that particular moment. Immune system fluctuates depending on the stressors.
Lymph nodes can swell and become tender during an outbreak.
The chance of tender lymph node enlargement is high during the first outbreak and lower during subsequent outbreaks.
What are lymph nodes?
Lymph nodes are tiny structures that filter infection and prevent its further development. Though lymph nodes are scattered throughout the body, in some areas these little structures are grouped together and responsible for the control of infectious processes in that region (they are called regional lymph nodes). These regions are the neck, armpits, abdomen, chest, and groin.
What is an enlarged lymph node?
“Enlarged” means bigger than normal size. It is not a feeling but rather a visible, palpable thing.
✓ In a herpes outbreak, regional lymph nodes become enlarged in response to infection.
- Oral herpes: neck and armpits lymph nodes
- Genital herpes: groin lymph nodes
✓ Lymph nodes usually become enlarged on the side of the skin lesion.
✓ Lymph nodes become enlarged during the early stages of a herpes manifestation (initial symptoms). They slowly return to the normal size within 2–4 weeks but usually persist longer than the visible signs of the disease.

PART 2
Photos of herpes symptoms in males and females
We present here some photos of herpes outbreaks borrowed from other websites. Seeing more outbreaks gives you the experience to begin noticing minor but important differences.
Let’s take a look at some photos of genital herpes in females and males so we can clarify what makes us think lesions are herpes and not something else.
These are the areas most commonly affected in males:
✓ Scrotum
✓ Penile shaft
✓ Penile head
✓ Foreskin
✓ Pubic area
These are the areas most commonly affected in females:
✓ Vulva
✓ Vagina
✓ Cervix
✓ Pubic area
Herpes photos for males
Warning
Contains sensitive content
View Gallery 7
![]() Herpes sores
Herpes sores
![]() Herpes sores
Herpes sores
![]() Herpes sores
Herpes sores
![]() Herpes sores
Herpes sores
![]() Herpes sores
Herpes sores
![]() Herpes sores
Herpes sores
![]()
Herpes photos for females

PART 3
Initial herpes outbreak
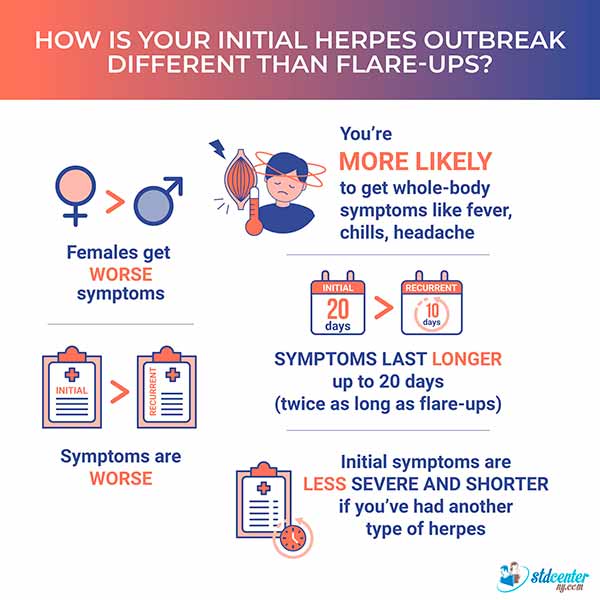
The symptoms of an initial herpes outbreak are more severe than those of flare-ups, and they last longer. Most likely, this is because the immune system is reacting to an unfamiliar virus. [7] Genital herpes simplex virus infections: clinical manifestations, course, and complications https://pubmed.ncbi.nlm.nih.gov/6344712/
The average duration of symptoms for an untreated initial outbreak is 20 days. New skin lesions might continue to develop for the first 5–7 days. [8] Genital herpes guide: Risk factors and clinical manifestations https://www.canada.ca/en/public-health/services/infectious-diseases/sexual-health-sexually-transmitted-infections/canadian-guidelines/herpes-simplex-virus/risk-factors-clinical-manifestation.html
Here are more important facts about an initial outbreak:
✓ The initial outbreak tends to be more severe in females.
✓ The chance of getting systemic symptoms like fever, chills, and headache is much higher with the first outbreak.
✓ The symptoms are less severe and shorter in people who have had another type of herpes.

PART 4
Recurrent herpes
After the initial outbreak, the herpes virus travels along nerves from the skin to the sacral ganglia (a bundle of nerves) in the spine and remain there, inactive, for some time. Once activated, the virus can travel from the ganglia back to the surface of the skin, causing a flare-up.
A herpes flare-up is usually milder (the symptoms are less severe) and shorter than the initial outbreak.
Where do recurrent herpes skin lesions appear?
Recurrent herpes skin symptoms might occur in exactly the same anatomic area as the initial outbreak, or close to it. Since the herpes virus stays dormant in the sacral ganglia and travels along nerves to the surface of the skin, any skin in the genital area innervated by the sacral ganglia (that is, any skin connected by nerves to the sacral ganglia) can undergo a flare-up. Therefore, it’s possible to have herpes flare-ups in the anal area without ever having anal sex.
How often should I expect herpes flare-ups, and what are the main factors affecting that?
Flare-ups may occur frequently in some patients. It depends on how strong their immune system is, how long they’ve had herpes, and the type of herpes virus (HSV-1 or HSV-2) affecting the area.
How does the immune system affect the frequency of herpes flare-ups?
The stronger the immune system, the less the chance of a flare-up. The immune system is weakened by illness, emotional stress, and certain medications.
How is the frequency of herpes flare-ups affected by disease duration?
Herpes is a regressive condition, which means the number of flare-ups and their severity decrease over time.
On average, about 71% of people will have at least one flare-up within the first year after the initial outbreak. The number of people who have a flare-up drops to 30% after the second year. [3] A guide for people with Herpes Simplex https://www.herpes.org.nz/application/files/7015/8138/6014/Herpes_The_Facts_2020_screen.pdf
The more severe the initial episode, the greater the chance of flare-ups, whether medication was taken or not.
The different herpes types (HSV-1 and HSV-2) have different recurrence rates.
Flare-ups of HSV-2 in the genital area occur more often than those of HSV-1. [4] Patient education: Genital herpes (Beyond the Basics) https://www.uptodate.com/contents/genital-herpes-beyond-the-basics
Around 80% of people with HSV-2 have one flare-up after the initial outbreak, while 50% of people with HSV-1 do.
And 35% of people with HSV-2 have frequent flare-ups.
Flare-ups of HSV-2 in the genital area occur more often than those of HSV-1. [5] Viral Shedding 1 Year Following First-Episode Genital HSV-1 Infection https://jamanetwork.com/journals/jama/fullarticle/2797619
Males with HSV-2 have about 20% more flare-ups than females—that explains the higher transmission rate from males to females. [6] Recurrence rates in genital herpes after symptomatic first-episode infection https://pubmed.ncbi.nlm.nih.gov/7978697/
How are recurrent herpes symptoms different?
Herpes flare-ups are shorter than the initial outbreak, lasting, on average 10 days (if not treated).
Recurrent herpes symptoms are more severe in females than in males.
Here are some random statistics
[7, 8]
Genital herpes simplex virus infections: clinical manifestations, course, and complications
https://pubmed.ncbi.nlm.nih.gov/6344712/
Genital herpes guide: Risk factors and clinical manifestations
https://www.canada.ca/en/public-health/services/infectious-diseases/sexual-health-sexually-transmitted-infections/canadian-guidelines/herpes-simplex-virus/risk-factors-clinical-manifestation.html
about herpes flare-ups that you may find interesting and helpful:
✓ 67% of people get significant systemic (whole-body) symptoms
✓ 25% of recurrent herpes episodes have no systemic symptoms
✓ 98% of people have local pain and itch
✓ 63% of people have pain with urination


PART 5
What herpes symptoms and signs do doctors consider reliable for establishing a diagnosis?
In diagnosing herpes, of most importance is whether these eight symptoms or characteristics are present:
1. Tingling of the skin and shooting nerve pain are occurring
Herpes rash can be preceded by a tingling sensation of the skin and localized shooting pain. This usually happens locally on the site of the skin rash.
When herpes virus enters the body through micro abrasions of damaged skin, it gets into nerve cells, where it permanently lives. Most of the time, the immune system keeps it suppressed and inactive
Tingling of the skin and shooting pain happens when the herpes virus is activated and travels along the nerve, inducing nerve firing.
2. The affected skin areas are thin and moist
Herpes rashes mostly affect the thin, moist skin areas of the genitals, such as the vulva and vagina for females and the penile head, scrotum, and shaft of the penis for males.
Why? Because it's easier to get microscopic cuts (micro abrasions) in those areas during sex, so the herpes virus can get through the skin more easily.
Herpes rashes can affect normal (thicker) skin areas, such as the pubic area, but that doesn't happen as often.
3. The area of the outbreak is very painful
Pain is a very common symptom of a herpes outbreak.
Herpes lesions (which be a bump, blister, or sore, depending on the stage of the disease) hurt all the time, but hurt even worse when they're touched.
The pain level is usually significant since the herpes sores in the genital area are irritated by walking and sitting.
4. The skin lesions are usually clustered
Herpes lesions are clustered-that is, located very close to each other, usually on the same red base.
One or two clusters of herpes bumps, blister, or sores can be seen, depending on the stage of the disease.
5. Only a superficial layer of skin is affected
Herpes lesions are very superficial, meaning they affect the very top layer of skin. They don't penetrate the entire skin thickness. So, with herpes lesions, the skin thickness is normal.
The skin thickness, or level of skin penetration by the rash, can be assessed visually (by looking) or with a "skin pinch test."
✓ When you look at the skin, you see skin that looks thicker or bumpier than neighboring skin.
✓ Using a "skin pinch test," you pinch the skin in the area of a lesion and compare it to the skin next to it. When the skin is "thicker," unlike with herpes, you can feel the induration (hardness) under your fingers.
6. The outbreak is usually one-sided
Herpes lesions are usually one-sided. This means that most of the time, the skin on only one side is involved: left or right. Occasionally, lesions are on both sides.
7. The skin lesions evolve, changing in appearance over time.
Herpes lesions usually evolve over time, going from one stage to another.
Herpes skin lesions don't stay in one stage for a long time; they evolve rapidly over a period of a week, on average (but this can take up to three weeks if it's a first outbreak).
The herpes rash starts as a redness. Then, bumps appear on the red skin; the bumps turn into blisters; the roofs of the blisters come off, forming sores; the sores become crusted; and the sores heal without leaving scars.
8. The lymph nodes swell.
Herpes lesions usually cause lymph node enlargement on the site of the rash.
Lymph nodes are usually enlarged locally (in the groin area) and might be painful to the touch.
Symptoms or signs: which is more reliable for the herpes diagnosis, and why?
Signs! They are objective because they can be seen and confirmed by people other than the patient. However, in the diagnostic process, even though doctors trust signs more, we consider both signs and symptoms and their timing to get a complete picture of what’s going on.
How reliable are herpes symptoms in establishing the herpes diagnosis?
Typically, a herpes diagnosis is established based on visual examination of the skin by an experienced healthcare provider. This is helpful because early treatment of the rash is possible.
Both signs and symptoms need to be considered in context: how soon after exposure they began, how they’re evolving over time (herpes goes through stages), whether there are any systemic symptoms, etc. Since most herpes symptoms are general and vague, they could be present not because of herpes but instead because of other medical conditions or even anxiety.
For a definitive diagnosis, HSV-1 and HSV-2 testing is advised. You can read here how to choose the right herpes test based on symptoms and timing.

9 reason it is genital herpes (HSV 2) and nothing else.
Source
- Fact Genital Herpes – CDC Detailed Sheet
https://www.cdc.gov/std/herpes/stdfact-herpes-detailed.htm - Kimberlin DW, Rouse DJ. Genital Herpes. N Engl J Med, 2004. 350(19): 1970–7.
https://www.nejm.org/doi/10.1056/NEJMcp023065 - A guide for people with Herpes Simplex
https://www.herpes.org.nz/application/files/7015/8138/6014/Herpes_The_Facts_2020_screen.pdf - Patient education: Genital herpes (Beyond the Basics)
https://www.uptodate.com/contents/genital-herpes-beyond-the-basics - Viral Shedding 1 Year Following First-Episode Genital HSV-1 Infection
https://jamanetwork.com/journals/jama/fullarticle/2797619 - Recurrence rates in genital herpes after symptomatic first-episode infection
https://pubmed.ncbi.nlm.nih.gov/7978697/ - Genital herpes simplex virus infections: clinical manifestations, course, and complications
https://pubmed.ncbi.nlm.nih.gov/6344712/ - Genital herpes guide: Risk factors and clinical manifestations
https://www.canada.ca/en/public-health/services/infectious-diseases/sexual-health-sexually-transmitted-infections/canadian-guidelines/herpes-simplex-virus/risk-factors-clinical-manifestation.html
Frequently Asked Questions
-
How long does a herpes outbreak last? Can I have a herpes outbreak for longer than a month?
Yes, you can, but that’s very unusual. It mostly happens to people who have a weak immune system:
- Immunosuppressive condition (such as AIDS or advanced cancers)
- Taking medication that might suppress the immune system (e.g., chemotherapy, heavy and prolonged steroid use)
In people with the above-mentioned conditions, outbreaks are more frequent and more severe in addition to being prolonged.
For most people, herpes sign and symptoms resolve within 2–4 weeks: longer with the initial outbreak and shorter with subsequent outbreaks. They also are less frequent and less severe as time goes on (it’s a regressive condition).
-
I have resolution of herpes symptoms. What does it mean?
Once you have herpes it will stay with you for the rest of your life and you can pass the infection to other people with and without symptoms.
Herpes virus does not get cleared by your immune system as many other viruses. It stays suppressed (latent form) in the local nerve ganglia and can resurface from time to time depending on the immune system at that moment.
So, if you believe you have had herpes symptoms and they got better, you can get a blood test for the HSV antibodies 3 months after the initial outbreak to get diagnosed officially.
-
I am 25 y.o male and have symptoms of genital skin burning/itching for a month. It (symptoms) is unchanged and constant. Skin is normal. Is it herpes causing my symptoms?
Based on the information we have it is very unlikely. Herpes symptoms usually followed by herpes signs in 1-2 days. The herpes outbreak usually goes through stages: symptoms, followed by signs appearance, followed by gradual resolution of the symptoms and signs. It is very unusual to be symptomatic for a month without having visible signs.
-
I am 27 y.o female and have been experiencing tingly felling around the vagina opening for 6 months. Everything started after I was notified by my ex that he is positive for the herpes. My herpes tests (multiple) never came back positive. Seen by multiple doctors (from neurologist to urologist), a lot of medical studies were done (MRIs of brain and lumbar spine, nerve conduction, CT scans, etc.) with normal results. They(doctors) all assumed it must be psychological. How can it be explained?
Sometimes the “symptoms” are just the result of your stress. Psychological cause for any disease can be established only after excluding other stuff. It cannot be considered as a first thing “off the bed”.
Why people develop psychological symptoms?
In case of herpes, this feeling usually appears after a risky (for that person) sexual intercourse (new partner, unprotected sexual act, and etc.).
It makes person uncomfortable, and person starts reading about all possibilities that can happen and start questioning if they have those symptoms.How doctors come to that (psychological reason) conclusion.
- Current symptoms should be carefully evaluated.
- Symptom and signs timing are important. Disease history can give a right context.
- Is it following the normal disease process? In this case, herpes process.
- Can other conditions give the same or similar symptoms? Rule them out with special testing and specialist evaluation.
- Psychological cause is assumed at this point.
-
I think I have herpes symptoms that aren’t progressing to visible signs. How common is that?
It is very unlikely that anyone will have symptoms of herpes that don’t evolve into signs.
- If you have symptoms (tingling and itch) and didn’t take any medication to stop the progression, herpes skin lesions should eventually appear. The time between symptoms and the appearance of the signs is called the prodromal period and it usually last from 12 hours to 2–3 days.
- Occasionally, the immune system is strong enough to suppress the progression of symptoms to signs, but in that case, symptoms should subside as well.
It is very unusual to have symptoms of itch and tingling in the area for weeks or months without progression to a visible stage of the disease.
-
I had my first genital herpes outbreak. A swab test confirmed that the skin lesion was herpes 2. I am symptom- free now. Where should I expect the next outbreak?
If the swab test confirmed HSV-2 in the genital area, the herpes virus will be suppressed by your immune system in that area. The next outbreak can happen anywhere in that area, not necessarily in the exact same place.
-
Can herpes cause urinary symptoms? How common is that?
Yes, it can. But it is uncommon.
Common urinary tract infection symptoms are burning, urgency, and increased frequency of urination. Since herpes causes the formation of sores, which can be on the outside of the vagina or urethral area, the most common symptom is burning while urinating. This burning pain might be pretty significant, and it is more common among women.
Occasionally, when blisters form inside the urethra, the patient might have difficulty with urination (expelling urine from the bladder) due to swelling of the urethra. -
Can penile or vaginal discharge occur with herpes infection? If so, what kind of discharge? Is it smelly?
Yes, one can get a discharge with herpes. Although this is not common and not specific to herpes, some people do experience it. There are some gender differences.
Herpes discharge in men
This discharge usually appears on the tip of the penis head. It occurs when the virus affects the urethra (in 35%–45% of infected symptomatic males). Typically, the penile discharge is whitish, thick, and clear. It may have a strong fishy odor, which is more noticeable during ejaculation. However, the odor is not as common as it is in females. In rare cases, the discharge may contain blood.
Herpes discharge in women
A vaginal discharge develops when the herpes virus affects the inside of the vagina. As with penile discharge, a vaginal discharge is whitish, thick, clear fluid that may contain blood.
Females are more likely to have a smelly (fishy) discharge than males. It is more noticeable after intercourse, which can cause the normal healthy bacteria of the vagina to be mixed with “unhealthy” bacteria or viruses (in this case the herpes virus).
Unlike with other vaginal infections that are well known for their odor (such as bacterial vaginosis, which has a fishy odor), doctors don’t rely on odor in diagnosing herpes.
-
Can herpes travel to other parts of the body on its own?
The herpes virus, once contracted, will stay dormant (inactive) in the nerve ganglion locally. It will not travel to any other part of the body unless you pass it to another area of the body (autoinoculation) during the outbreak, which is extremely uncommon. An example of this is touching the active sore and immediately touching another part of the body.
Herpes remains local (in the area of exposure), and when certain triggers activate the virus, you may have an outbreak in the area of exposure (oral or genital). It might not be in the same exact spot as during the last outbreak.

By Slava Fuzayloff. D.O
Dr. Slava Fuzayloff is practicing STD physician with 20 years of experience and expert writer in the field of the sexually transmitted diseases.

